Key Facts:
- Traces of vaccine-derived poliovirus were detected in London sewage water samples in June 2022.
- No new cases of polio are known to have been reported in the United Kingdom as of this publication, but the level of viral presence in the sewage suggests that there may be local spread.
- It is not believed to pose a risk to the public at this time. Health authorities have declared a national incident and are investigating whether there is a greater health and safety concern.
- Social media posts attempting to sow doubt and confusion about the safety and efficacy of vaccines in the wake of the discovery are based on misinformation.
- Immunization remains the best protection against any of the four strains of polio infection, according to health authorities.
In June 2022, British health authorities found traces of vaccine-derived poliovirus in London sewage water — a finding that, in itself, is not necessarily uncommon. Each year, between one and three “vaccine-like” polioviruses are detected in the country’s water. What’s different in this case, however, is that the amount of virus present in the water suggests that there may be community-level spread, which has prompted the U.K. Health Security Agency (UKHSA) to declare a national incident.
Some conspiratorial-minded social media users took advantage of the announcement to speculate about the dangers of vaccine shedding and spread the inaccurate claim that immunizations — including those that offer protection against COVID-19 — not only don't work, but present a health hazard to the public in and of themselves. BBC reporter Shayan Sadarizadeh compiled a handful of examples and shared them to Twitter:
Confusion about "vaccine shedding" (or, more properly, "viral shedding") as a mechanism for the spread of disease has cropped up before in recent years, specifically in unfounded claims regarding the safety of COVID-19 vaccines. The bottom line is this: To make such broad claims implicating vaccines in the spread of disease overgeneralizes the specifics of two very different vaccination and immunization programs.
To fully understand the scientific nuances at the center of London's poliovirus scare, let's first understand the virus itself.
What Is Polio?
Just a century ago, polio was a common infection with lifelong effects. Perhaps most famously, Franklin D. Roosevelt, the 32nd U.S. president, was diagnosed with polio at the age of 39 and experienced difficulty walking for the rest of his life. By the late 1940s, polio outbreaks in the U.S. had increased in frequency and affected about 35,000 each year.
Poliovirus is considered largely eradicated globally, with the exception of two countries: Pakistan and Afghanistan, though a case linked to Pakistan was detected in Malawi, Africa, in February, according to the Polio Global Eradication Initiative (PGEI). But cases do arise, particularly in regions with low immunization rates. About 1 in 4 people infected with poliovirus will experience symptoms, which the Centers for Disease Control and Prevention (CDC) says will most include sore throat, fever, fatigue, nausea, headache, or stomach pain. Extreme cases — about 1 in 100 — may experience feeling of pins and needles in the legs, meningitis, or paralysis in parts of the body.
Types of Polio Vaccine and How They Are Administered
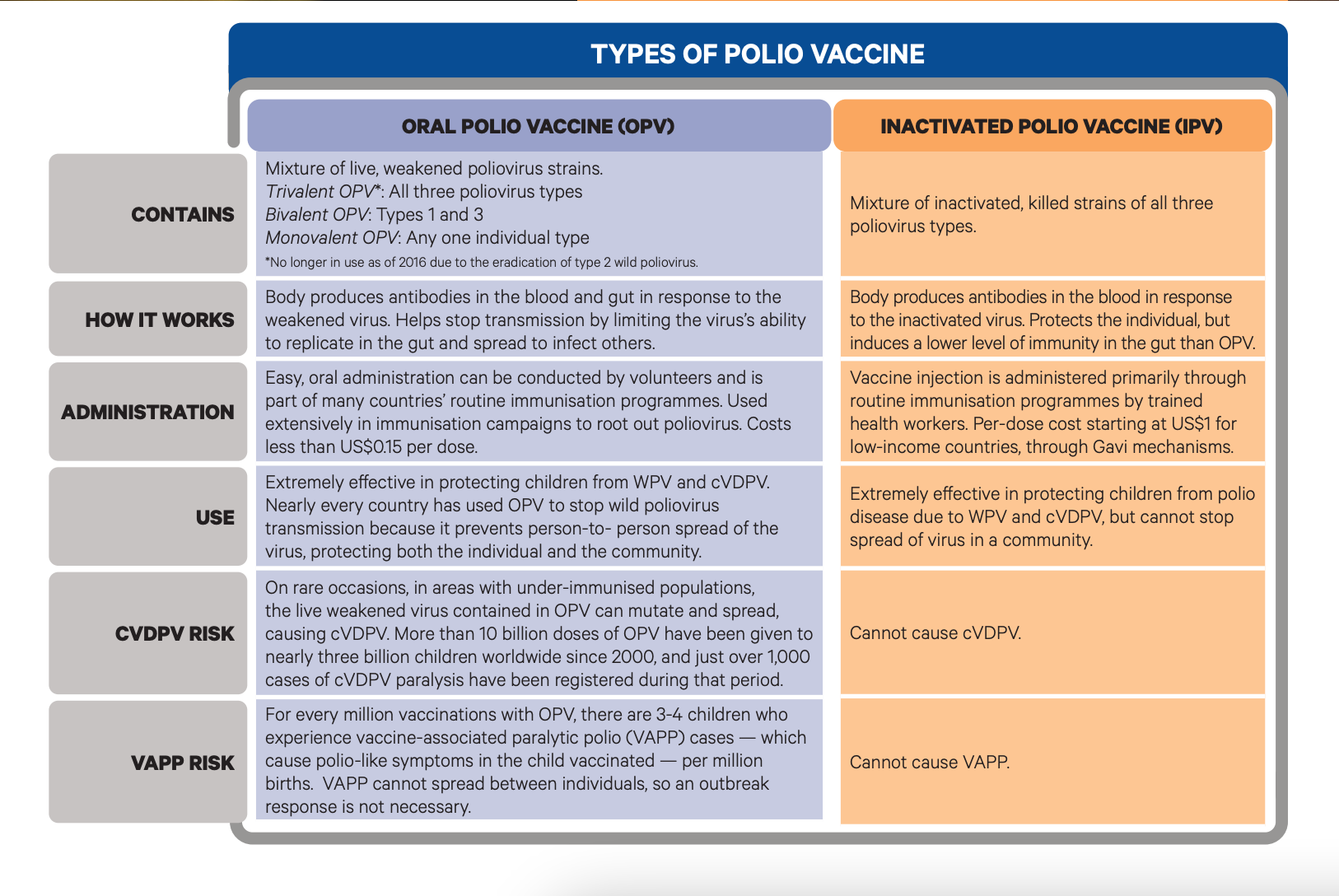
There are four known types of polio vaccines in circulation, three of which are wild strains and one that can be caused by a mutated virus from the oral polio vaccine (OPV). In addition to OPV, there are three other types of vaccinations:
- Monovalent Oral Polio Vaccine Type 2 (mOPV2) that offers protection against one strain.
- Novel Oral Polio Vaccine Type 2 (nOPV2) that is more genetically stable.
- Inactivated Polio Vaccine (IPV) that offers protection against the three wild strains and is the only polio vaccine currently administered in the U.S. and most high-income nations.
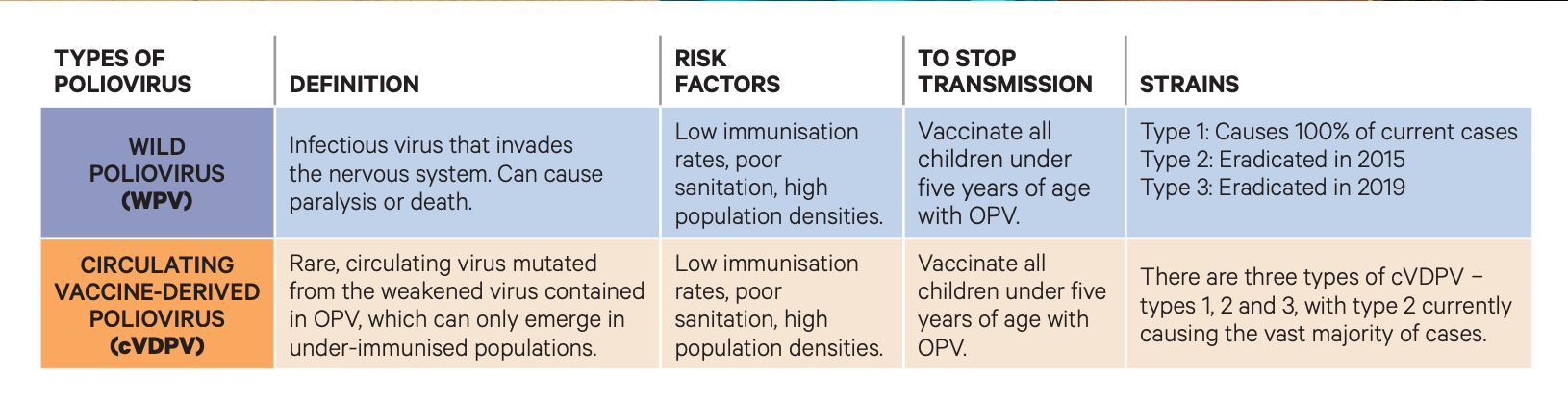
The wild variants of poliovirus cause a highly infectious viral disease that can invade the nervous system and cause paralysis.
Wild poliovirus is the most common form of poliovirus and while cases of vaccine-derived poliovirus (cVDPV) are rare, numbers have been increasing in recent years because of low immunization rates in communities. In 2020, there were 959 reported cases of cVDPV type 2 globally, notes PGEI.
As its name suggests, oral polio vaccine is administered via droplets in the mouth. OPV is what is known as a "live attenuated vaccine" and contains a weakened sample of a virus that, when exposed to a person, stimulates a live response so that the body can develop antibodies. OPV played a role in eradicating polio globally and reduced wild polioviruses by 99.9% since 1988. Rarely, however, a live attenuated vaccine can trigger disease in a recently vaccinated person.
Sometimes, if a live and weakened strain from OPV circulates long enough in a community it can mutate to cause the type of polio known as cVDPV — this is not a reemergence or indication of wild polio but rather a rare occurrence of a mutated strain. Though OPV is recognized as a key challenge to eradication efforts, in many cases the potential, rare risk of cVDPV in a community is far outweighed by the larger goal of eradicating of wild polio.
“However, in communities with low immunization rates, as the virus is spread from one unvaccinated child to another over a long period of time (often over the course of about 12-18 months), it can mutate and take on a form that can cause paralysis just like the wild poliovirus. This mutated poliovirus can then spread in communities, leading to cVDPVs,” wrote the Polio Global Eradication Initiative
Cases of cVDPV infection mainly occur in places with overall low vaccination rates, particularly poorer regions, regions experiencing civil conflict, and places where people are experiencing vaccine hesitancy due to misinformation. Because cVDPVs can be spread through stool, communities with low sanitation may also see higher incidences. Additionally, during the COVID-19 pandemic, routine healthcare programs were disrupted and large-scale polio campaigns were suspended from March to July 2020, creating immunity gaps that led to new outbreaks and further increased transmission of cVDPV globally.
Polio Vaccinations Today
Because it is given by mouth, OPV is easy to administer in places lacking in healthcare and is the first step in eradicating wild polio. Once wild polio is deemed eradicated from an area, healthcare experts switch to IPV (inactivated polio vaccine), which offers protection against both wild polio and cVDPV.
IPV vaccines are given in high-income nations like the U.S., where it has been the only polio vaccine since 2000. IPV is typically given over the course of four doses in children at 2 months old, 4 months old, 6 through 18 months old, and 4 to 6 years old, according to the CDC. Because most adults should be fully vaccinated against polio via IPV, protection is likely to be widespread (but there are exceptions such as those traveling to a country at-risk of infection or some healthcare providers).
Though cases of cVDPVs are rare in nations like the U.S., they’re not unheard of. In 2005, vaccine-dependent poliovirus was found in the stool of an unvaccinated child with a weakened immune system in Minnesota who likely caught it by coming into contact with someone who had received the OPV in another country while traveling two months prior. After their diagnosis, seven unvaccinated children in the same community had poliovirus, none of whom experienced paralysis. That same year, unimmunized young adults from U.S. contracted VAPP in Central America, likely from the infant grandchild of a host family who had been recently immunized with OPV.
In 2009, an adult with a weakened immune system developed VAPP and died of complications. It was an isolated event.
In 2013, a severely immunocompromised infant died after receiving OPV in India.
Presence of Vaccine-Derived Poliovirus in London, June 2022
First and foremost, as of this writing, there are no known human cases of vaccine-derived poliovirus confirmed in London. Rather, traces of one strain of the virus, type 2 vaccine-derived polio that can be shed through fecal matter, had been identified in city sewage water in North and East London between February and May. Genetic analysis indicates that there is likely spread between closely linked individuals. As The New York Times reported, health authorities declared it a national incident because there is the possibility of local spread of this vaccine-derived polio (more on what that means below).
“The virus has continued to evolve and is now classified as a ‘vaccine-derived’ poliovirus type 2 (VDPV2), which on rare occasions can cause serious illness, such as paralysis, in people who are not fully vaccinated,” wrote the UKHSA. As of this publication, the World Health Organization (WHO) reports that there are no cases of paralysis, a rare symptom that can be present in extreme cases of VDPV2, and contends that there is no risk to the public health.
The last known wild polio case (which is separate from vaccine-derived polio) in the U.K. was reported in 1984 and declared eradicated in 2003. In London currently, it is estimated that 86.6% of the population is immunized. Health officials are continuing to monitor and determine the source of infection and emphasize the importance of being fully vaccinated against poliovirus.
What Are 'Vaccine Shedding' and 'Viral Shedding,' and How Do These Relate to COVID-19 Immunizations?
As we have previously reported, there is no evidence to suggest that individuals vaccinated against COVID-19 can shed viral components (for example, DNA) that are capable of infecting and harming those around them (this was the sense in which some anti-vaccination rumor-spreaders used the term "vaccine shedding." Viral shedding, by contrast, occurs when an infected person sheds actual virus particles from their nose and mouth.
“cVDPVs can emerge if the weakened live virus contained in oral polio vaccine, shed by vaccinated children, is allowed to circulate in under-immunized populations for long enough to genetically revert to a version that causes paralysis,” writes PGEI. In “sporadic and rare” incidencts, cVDPVs can cause vaccine-associated paralytic poliomyelitis, or VAPP.
While it is true that live attenuated vaccines (such as OPV) can sometimes cause shedding, none of the COVID-19 vaccines approved or authorized for use in the U.S. contains a live virus. Rather, mRNA vaccines like Comirnaty (formerly Pfizer-BioNTech) and Moderna use a piece of DNA known as the mRNA as a signal to the body to teach the immune system to recognize and identify SARS-CoV-2 in the event of an infection. mRNA is not a live virus.
“After making the protein piece, cells display it on their surface. Our immune system then recognizes that it does not belong there and responds to get rid of it,” wrote the CDC. “When an immune response begins, antibodies are produced, creating the same response that happens in a natural infection.”
Vaccine-Derived Poliovirus is Certainly Not Evidence for COVID-19 Vaccine Shedding
Poliovirus vaccinations and those used against COVID-19 use different medical strategies to provide protection against disease. While vaccine-derived poliovirus can spread through contact between recently OPV-immunized people — either through respiratory droplets or exposure to feces — the highest risks are present in communities that have low vaccination rates. For the best protection against any of the four strains of poliovirus, health officials contend that IPV immunization is the most efficient.
In sum, differences between polio and covid vaccines make informal comparisons between the two useless. There are important differences between the types of polio vaccines available and when each is administered, compared with existing COVID-19 vaccines. Vaccine-derived poliovirus is known to occur, rarely, after vaccinations using one type of vaccine, oral polio vaccine (OPV), which is only administered under certain circumstances.